HEALTHY INDOOR MICROBIOME – AN INTRODUCTION

ABSTRACT/SYNOPSIS
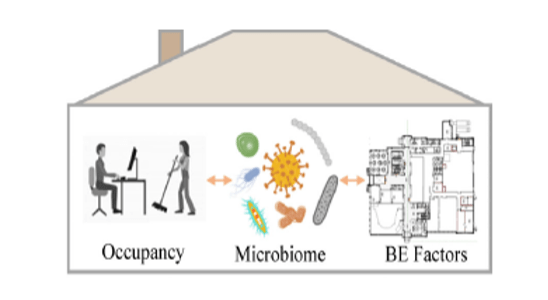
Indoor air quality constitutes as one of the major factors in development and maintenance of overall well-being/good health of humans. It refers to the quality of the air in any anthropogenic or built environments (BE) such as homes, schools, offices, financial institutions like banks, childcare facilities, etc. as demonstrated in Figure 1. Indoor air quality varies a lot on the category of living organisms inhabiting within a given environment. The collective sum of all the living organisms and their by-products within the environment are known as Indoor Microbiome. The term “Indoor Microbiome” includes a broad spectrum of living microorganisms such as bacteria, virus, fungi, unicellular organisms like algae, protozoa, etc. and non-living microbial components and byproducts of microbial metabolism such as volatile organic compounds. A vast majority of our time is spent indoors, especially since the onset of the Covid-19 pandemic where the percent of employed population working from home nearly doubled. Recent studies by the US EPA have shown that Americans spent approximately 90 percent of their time indoors. These statistics give us an insight into understanding the level of human exposure to microbiomes in anthropogenic environments, the impact of these exposures, and give the required momentum to modify these environments to potentially impact human health and overall well-being.
Microbiomes of the built environment or anthropogenic environments have a significant impact on human health. Microbes are responsible for over 400 million lives annually (Fitzpatrick et.al. 2019), some of which are due to the transmission of microbes via air and surface contact in the built environment causing several illnesses including the ongoing Covid-19 pandemic. Although, most microbes are associated with transmission of diseases, not all microbes are detrimental to the human health. Many researchers and scientists are now becoming increasingly aware of the role of “healthy” or “beneficial” microbes that play a significant role in preventing diseases. This article provides an overview of what constitutes a “healthy” indoor microbiome and characteristics and benefits of indoor microbiomes. This article is part of new series by Sani Service titled “Microbiome of the Built Environment” that provides an understanding of the microbes residing in the built environment or anthropogenic environments such as residential houses, office buildings, schools, etc., sources of microbes, impact of microbes on human health, and factors contributing to the growth of microbiomes in the built environment. Sani Service are one of the leading providers in excellent and sustainable indoor air quality treatment solutions for both residential and commercial clients.
CHARACTERISTICS AND BENEFITS OF A “HEALTHY” INDOOR MICROBIOME
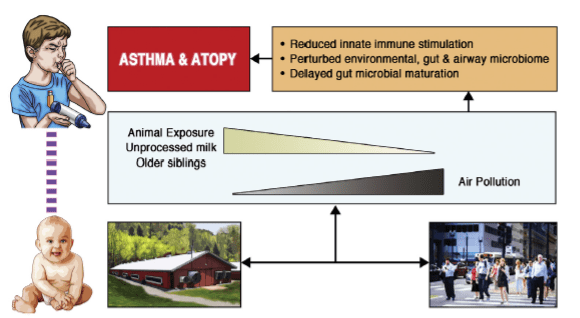
The primary definition of “healthy” indoor microbiome is the type or class or microorganisms that not only help prevent diseases but also promote overall well-being in humans. Several studies have shown the association between healthy indoor microbes and disease prevention, particularly reducing risk of asthma among children who grow up in farms or households with proximity to cattle and livestock. The studies indicated that home dust from areas near farm/livestock contains microbiota characterized by high bacterial growth and some quantities of microbes associated with cattle that helps in prevention and protection from allergies and asthma attacks particularly in young children who are prone to infections owing to a developing immune system and high percentage of time spent in dirt/floor while playing. These useful farm bacteria can be used to model healthy indoor microbes which can be cultivated and grown in residential houses that are not necessarily near farms. Figure 2 provides a graphical representation of this association between different built environments and the role of healthy indoor microbes in preventing diseases in children.
Figure 2. Simplified Association Between Urban vs Rural Built Environment and Likelihood of Asthma and Atopy
Another research study demonstrated that home dust in houses with dogs could potentially improve respiratory immunity to allergens, pollen, and other airborne contaminants. These studies indicate that “healthy” microbiomes could be incorporated into design of buildings and structures to help promote exposure to beneficial microbiomes for overall well-being.
However, the characteristics or components of a healthy indoor microbiome are much complex and need thorough research and deeper understanding of the diverse functions of microbes. Microbial interaction with the human body occurs simultaneously with exposure to allergens, pollutants, and chemicals. Additionally, the impact of all these agents can vary depending on the nature of the population such as age, gender, diet, existing health conditions, etc. Further studies and research is needed in this area to evaluate and classify indoor microbes as “beneficial indoor microbes”.
REFERENCES
- Dannemiller, K. C. (2019). Moving towards a robust definition for a “healthy” indoor microbiome. Msystems, 4(3), e00074-19.
- National Academies of Sciences, Engineering, and Medicine. (2017). Microbiomes of the built environment: a research agenda for indoor microbiology, human health, and buildings.
- Gilbert, J. A., & Stephens, B. (2018). Microbiology of the built environment. Nature Reviews Microbiology, 16(11), 661-670.
- Li, S., Yang, Z., Hu, D., Cao, L., & He, Q. (2021). Understanding building-occupant-microbiome interactions toward healthy built environments: A review. Frontiers of environmental science & engineering, 15(4), 1-18.
- Fitzpatrick, M. C., Bauch, C. T., Townsend, J. P., & Galvani, A. P. (2019). Modelling microbial infection to address global health challenges. Nature microbiology, 4(10), 1612-1619.
- Lee-Sarwar, K. (2021). The farm-like effect: Rural exposures in early life, the microbiome, and asthma. Journal of Allergy and Clinical Immunology, 148(1), 89-90.
- //www.epa.gov/indoor-air-quality-iaq/indoor-microbiome
- //www.epa.gov/report-environment/indoor-air-quality#note1
By Abhiram Satyadev